-
Články
- Časopisy
- Kurzy
- Témy
- Kongresy
- Videa
- Podcasty
Early Experiences Implementing Pre-exposure Prophylaxis (PrEP) for HIV Prevention in San Francisco
article has not abstract
Published in the journal: Early Experiences Implementing Pre-exposure Prophylaxis (PrEP) for HIV Prevention in San Francisco. PLoS Med 11(3): e32767. doi:10.1371/journal.pmed.1001613
Category: Health in Action
doi: https://doi.org/10.1371/journal.pmed.1001613Summary
article has not abstract
Summary Points
-
Pre-exposure prophylaxis (PrEP) has been demonstrated to be safe and efficacious in clinical trials and emtricitabine/tenofovir was approved by the United States Food and Drug Administration for use as PrEP in 2012.
-
We report early experiences with PrEP uptake and delivery in three different settings in San Francisco: a PrEP demonstration project in a municipal sexually transmitted diseases (STD) clinic, and two PrEP delivery programs (a private health maintenance organization and an HIV-specific reproductive health program).
-
Interest in PrEP is high in San Francisco, particularly among men who have sex with men attending the STD clinic, and it is feasible to incorporate PrEP into busy clinical settings. Key next steps for PrEP implementation include increasing PrEP knowledge; expanding PrEP access; combating PrEP stigma; and optimizing interventions to promote PrEP uptake and adherence while reinforcing risk reduction strategies.
-
PrEP can be an important component of a comprehensive HIV prevention program and complement efforts to increase HIV testing, linkage to care, and early initiation of antiretroviral therapy.
PrEP: Opportunities and Challenges
In July 2012, more than 30 years after the initial HIV case reports, the United States (US) Food and Drug Administration (FDA) approved the first drug for the prevention of sexually acquired HIV infection. On the basis of compelling safety and efficacy data from pre-exposure prophylaxis (PrEP) trials of men who have sex with men (MSM) conducted across four continents and serodifferent heterosexual couples and young men and women in sub-Saharan Africa [1]–[3], the FDA issued the landmark approval of once-daily, co-formulated emtricitabine/tenofovir (FTC/TDF) for HIV prevention in men and women at risk for acquiring HIV infection through sexual exposure. Another recent trial showed PrEP was safe and efficacious in injection drug users in Thailand [4]. PrEP trial results highlight the critical relationship between adherence and efficacy [5], the lack of risk compensation in blinded PrEP trials [2],[6],[7], and the importance of ensuring individuals are HIV-negative prior to initiating PrEP to minimize HIV resistance [8]. Furthermore, modeling studies suggest PrEP can be a cost-effective HIV prevention strategy, particularly if targeted to the highest risk populations [9]–[11].
Although the FDA approval marks an important milestone in HIV prevention, several factors, including negative results from two recently completed PrEP trials among women in Africa [12],[13]; perceived low demand for PrEP [14]–[17]; and concerns about drug adherence [18], spread of antiretroviral resistance [19], medication diversion [20], risk compensation [21], and cost [22] have led to debate on whether and how PrEP should be implemented [23]–[30]. The World Health Organization has issued guidance recommending PrEP demonstration projects be conducted to address these important issues and help determine how PrEP may best be scaled up in different settings to maximize public health impact [31], and a number of PrEP demonstration projects and roll-out programs are being planned or are underway [32]. We describe early experiences with PrEP uptake and delivery in the first year of PrEP implementation post-FDA approval in three different settings in San Francisco, California: an NIH-funded PrEP demonstration project in a municipal STD clinic and two PrEP delivery programs (a managed care organization and a HIV-specific reproductive health clinic). We also propose next steps for the prevention field based on insights learned from our early experiences with PrEP implementation.
Moving from Efficacy to Effectiveness
On the basis of promising efficacy data from PrEP trials, programs to evaluate PrEP delivery launched in San Francisco, a metropolitan area heavily impacted by HIV, with an HIV prevalence of 23% among MSM [33] and an estimated incidence of 782 cases/100,000 MSM (95% CI 505–1,058) in 2011 [34]. These programs are directly assessing concerns about uptake, adherence, resistance, and risk compensation, as well as models of PrEP delivery in different settings. We describe the core components of these varied programs (see Table 1), present preliminary data on PrEP uptake in these three programs, and summarize lessons learned to date.
Tab. 1. Core components of PrEP delivery programs in San Francisco. 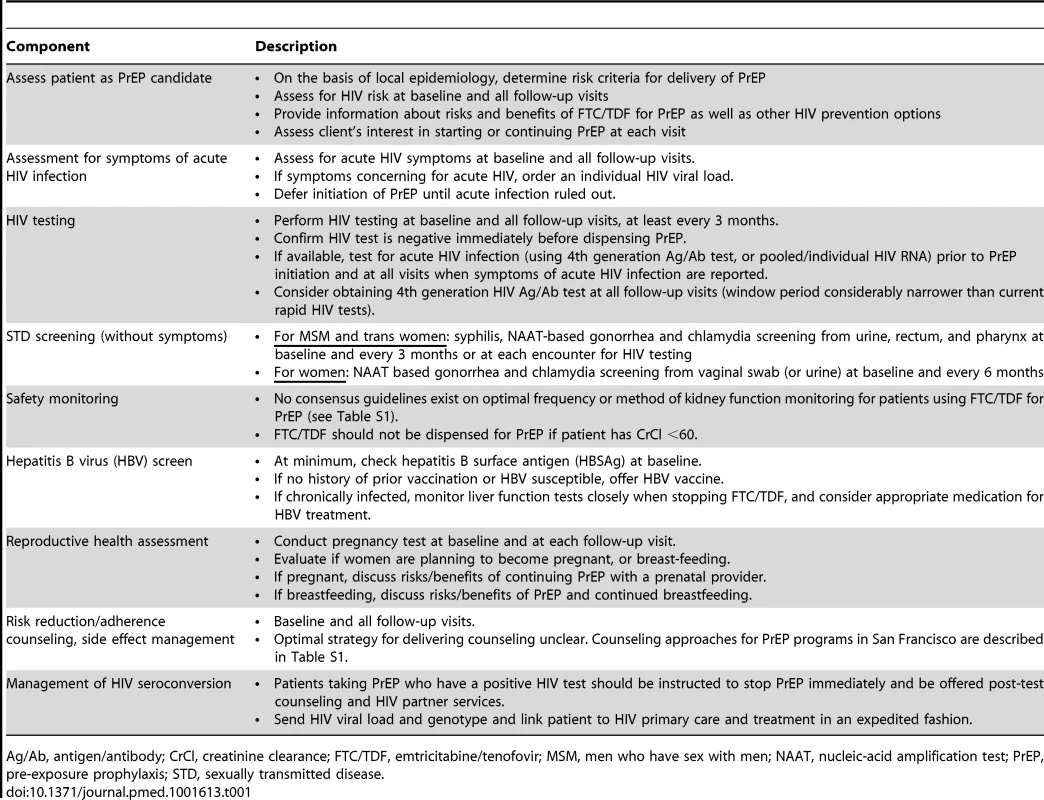
Ag/Ab, antigen/antibody; CrCl, creatinine clearance; FTC/TDF, emtricitabine/tenofovir; MSM, men who have sex with men; NAAT, nucleic-acid amplification test; PrEP, pre-exposure prophylaxis; STD, sexually transmitted disease. PrEP in an STD clinic
San Francisco City Clinic (SFCC), the city's municipal STD clinic, offers a range of sexual health services, including HIV and STD screening, diagnosis and treatment, HIV post-exposure prophylaxis (PEP), family planning, and emergency contraception. In 2011, the clinic conducted approximately 19,000 visits with 12,000 patients, of whom 38% were MSM and 1% transgender. HIV incidence among MSM at SFCC is high, with a 2.3% annual seroconversion rate [35]. In October 2012, SFCC began offering PrEP to MSM and transgender women through The Demo Project, a one-year National Institutes of Allergy and Infectious Diseases-funded PrEP demonstration project (Table S1).
From September 2012–2013, 571 individuals have been evaluated at SFCC for PrEP, and 261 participants have enrolled in The Demo Project, for an overall uptake of 49% among potentially eligible clients (Table 2). The most common reasons for declining PrEP include not enough time for study participation (28%), side effect concerns (25%), and no perceived HIV risk (8%). PrEP uptake appears higher among those with prior knowledge about PrEP and those reporting higher risk behaviors. Demand for PrEP has exceeded clinic capacity, with a wait-list of several dozen clients. To date, overall study retention is high; approximately 8% of participants have discontinued PrEP (Table 3). Several participants have expressed anxiety about PrEP access after completing their one-year participation in this project. Project staff are identifying sources of PrEP in the community, linking participants to prevention and care upon project completion.
Tab. 2. PrEP uptake and follow-up in three PrEP delivery programs in San Francisco. 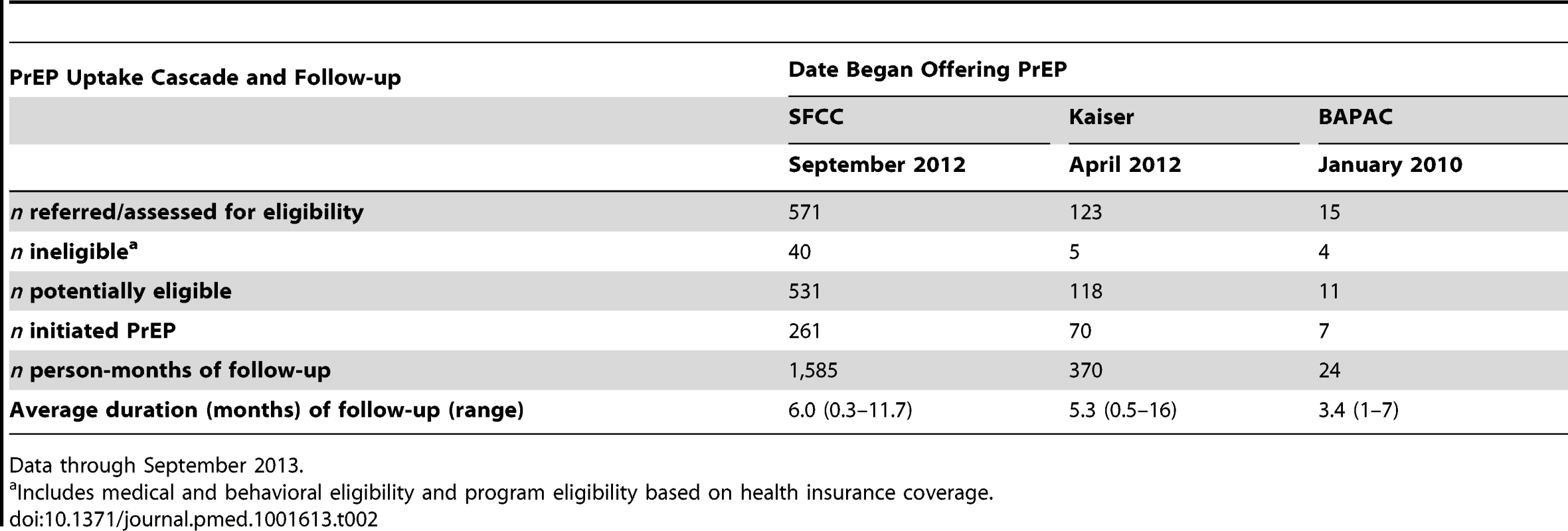
Data through September 2013. Tab. 3. Reasons for discontinuing PrEP across three PrEP delivery programs in San Francisco. 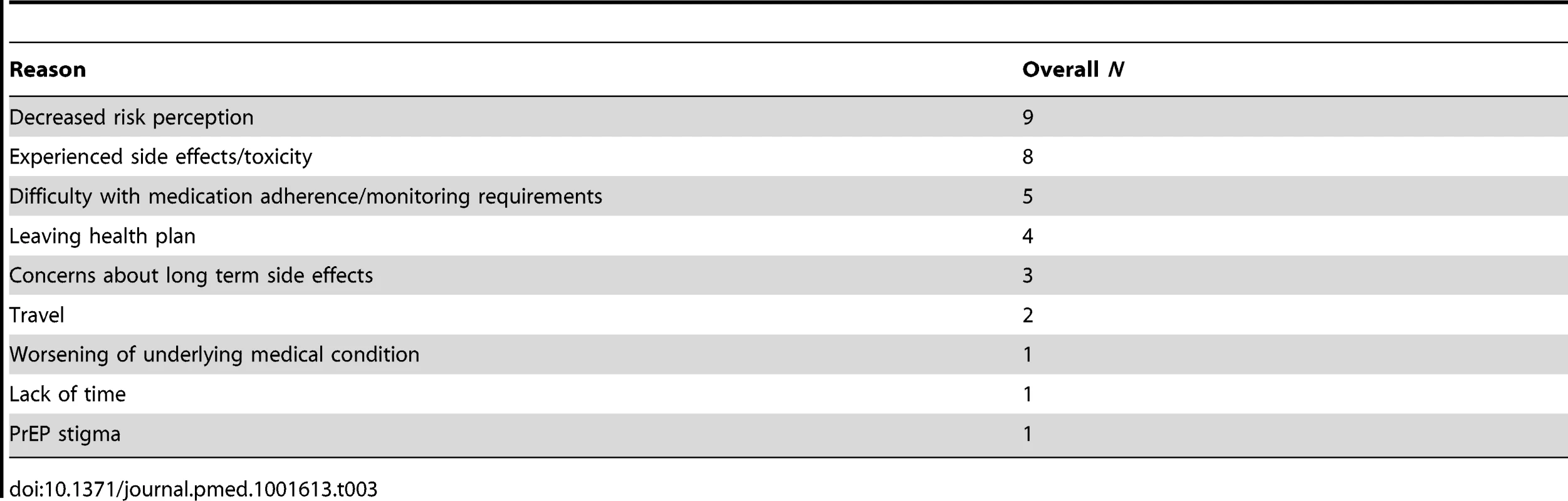
PrEP-related stigma (participants feeling stigmatized by others regarding their decision to use PrEP) has deterred some clients from accessing PrEP. Participants in the Demo Project are asked quarterly about social harms related to study participation. Fifteen of 20 social harms reported to date were related to PrEP stigma. Participants reported stigma from peers, who believe that PrEP will lead to increased risk-taking behavior and may divert resources away from HIV-positive people, and medical providers, who are unwilling to prescribe them PrEP or appear judgmental about their decision to use PrEP.
PrEP in a health maintenance organization
Kaiser Permanente Health Plan provides comprehensive primary and specialty medical care to over 185,000 members in San Francisco. More than 2,500 HIV-positive adults receive care through Kaiser's HIV Care and Prevention Program. Health plan members have a broad spectrum of payor sources for access to Kaiser insurance, including employer-based programs, Medi-Cal, and Healthy San Francisco (a health access program for low income residents of San Francisco) [36]. In May 2012, a PrEP program was initiated in conjunction with other routine HIV prevention strategies (Table S1). Although HIV medication prescribing is restricted to HIV specialists, all adult primary care providers are encouraged to refer interested individuals to the HIV program coordinators, either a pharmacist or nurse, for possible initiation of PrEP. While the number of patients who discuss PrEP with their providers and decide not to pursue a referral is not systematically captured, informal discussions with providers with large panels of MSM suggest that for every person referred, one to three members declined referral after a discussion about PrEP with their provider.
Since the launch of the Kaiser's PrEP program in San Francisco in April 2012, more than half of the 123 men and women referred by both HIV-specialty providers (65%) and non-HIV-specialty providers (35%) have initiated PrEP (table 2). Most common reasons for declining PrEP include decision to use PEP (47%), failure to respond to intake request or initial lab testing (28%), and underlying medical conditions (11%). Of those started, approximately 24% have discontinued FTC/TDF due to a variety of reasons (Table 3).
PrEP in an HIV-specific reproductive health program
Bay Area Perinatal AIDS Center (BAPAC) is a program of the University of California San Francisco, providing comprehensive preconception management and prenatal care to HIV-positive women and HIV-negative women with HIV-positive male partners (Table S1). BAPAC manages approximately ten to 15 HIV-positive pregnant women and provides preconception counseling for eight to ten patients per year. Potential candidates for PrEP are referred to BAPAC by local providers or are self-referred for consultation on lowering HIV transmission risk during conception and pregnancy. In 2010, BAPAC began offering PrEP to HIV-negative pregnant women who were having sex without a condom with HIV-positive male partners. In 2012, BAPAC expanded the PrEP program to include HIV-uninfected women seeking safer conception options with their HIV-infected male partners. BAPAC has also recently launched the PRO-Men initiative to educate HIV-positive men who have sex with women about their reproductive options and provide preventive services to their HIV-negative female partners, including PrEP. BAPAC provides care for women through six weeks post partum, when women transition to a primary care provider who can continue to prescribe PrEP as needed.
Since 2010, 15 HIV-negative women with HIV-infected male partners have been screened as part of comprehensive HIV prevention counseling at BAPAC for PrEP eligibility. Seven of these women initiated PrEP during prenatal or preconception care, one of whom stopped PrEP after a few days due to nausea and low risk perception given her partner's long term viral suppression. Reasons for not initiating PrEP included lack of insurance coverage, and a combination of low risk perception, concerns about risks to themselves or their babies, and cessation of risk behavior.
While only a few women have initiated PrEP at BAPAC thus far, data suggest HIV-serodifferent couples in the US want to incorporate PrEP as a safer conception option. Between 2006 and 2011, the National Perinatal HIV Hotline and Clinicians' Network took 152 calls regarding conception for serodifferent couples; the volume of calls has increased over time, from ten calls in 2006 to 43 in 2011 [37]. Thirty-four percent of callers sought advice specifically on alternative safer conception interventions such as timed intercourse and PrEP.
Key Lessons Learned
Lessons learned from three San Francisco PrEP programs can inform future PrEP rollout. First, accurate consumer knowledge about PrEP is a critical first step in PrEP implementation, and prior PrEP awareness was associated with increased uptake in the STD clinic setting. Second, across all three programs, patient risk perception and concern about side effects appear to play an important role in PrEP uptake, adherence, and persistence (continuing PrEP over time) and will need to be addressed to optimize PrEP targeting and implementation. Third, ensuring adequate clinic capacity and sustainable delivery of PrEP is critical to addressing ongoing high demand for PrEP. For time-limited PrEP programs (e.g., Demo Project and BAPAC), it is important to create linkage to ongoing PrEP access after program completion. While this may be a lesser concern for PrEP programs embedded within existing clinical systems (e.g., Kaiser), insurance coverage for PrEP is an important consideration in determining ongoing PrEP access across all programs. Finally, PrEP stigma can pose a barrier to uptake and retention and will need to be addressed among both providers and communities to maximize the impact of PrEP.
Next Steps for PrEP
On the basis of these lessons learned, we have identified priority next steps to address emerging delivery issues and to maximize PrEP's public health impact. While the examples provided focused on PrEP implementation in the US, several of these concepts and principles may be generalizable to PrEP delivery outside of the US.
Increase PrEP knowledge
Increasing PrEP knowledge among potential PrEP users is a key step to facilitating PrEP implementation [38]. Community awareness of PrEP appears to be increasing in San Francisco, with PrEP awareness increasing from 20% in 2006 [39] to 44% in 2011 in community-based surveys (Raymond H Fisher, personal communication, September 27, 2013). Increasing PrEP awareness is likely due in part to a range of community engagement activities conducted in collaboration with community partners. For example, co-incident with the initiation of the Demo Project, the San Francisco AIDS Foundation launched a broad PrEP education campaign, including ads on billboards and in transit stations and an informational website (prepfacts.org). Several well-attended public discussion forums were also held in the community. PrEP knowledge among individuals at-risk for HIV has been limited across the US [40] but appears to be slowly increasing after release of iPrEx results [17],[41]. In recent surveys of PrEP knowledge, PrEP awareness ranged from 19% in an online sample of US MSM [17] to 63% among serodifferent couples in San Francisco [15]. Another challenge is that individuals who could benefit from PrEP are often not engaged in care. Collaboration with community partners outside of clinic settings will be critical to reaching at-risk populations, providing PrEP education, and facilitating linkages to PrEP providers [32].
Expand PrEP access
As interest in PrEP among high seroincidence populations continues to rise in San Francisco, additional PrEP delivery sites in the community are needed. Increasing access to PrEP requires ensuring patients have affordable access to FTC/TDF. Some commercial private insurers are providing coverage for PrEP, although co-pays vary by plan, and some insurers may require prior authorization [42]. The rapidly changing health insurance marketplace, including implementation of the Affordable Care Act, may change PrEP access in as yet unknown ways. Currently, Gilead provides uninsured patients access to FTC/TDF through their medication assistance program [43].
Developing a cadre of skilled providers will also be essential to scaling up PrEP [44]. Many individuals do not feel comfortable discussing risk behaviors with their providers [45],[46], and many providers do not initiate discussion about HIV risk with their patients [47]–[49]. Providers may not have experience prescribing or monitoring patients taking FTC/TDF. Increasing PrEP knowledge among health care providers and identifying and training community providers who are skilled in taking sexual histories and prepared to offer PrEP as part of a comprehensive prevention package will be critical to expanding PrEP access.
PrEP delivery systems will also need to accommodate the increased visit volume associated with scaling up comprehensive PrEP services. PrEP delivery is feasible, but requires staff, time, space, and expertise. A range of models for PrEP delivery have been proposed, including STD clinics [38], primary care clinics [50], and community-based organizations with co-located or linkage to clinical services [51], although each of these settings may face unique challenges in PrEP delivery. For example, while STD clinics serve a population at-risk for HIV infection, most operate on a drop-in or urgent care basis and do not have established systems for providing continuity care or ongoing monitoring (e.g., creatinine testing). Conversely, primary care clinics are experienced with continuity care, but will require approaches to identify patients eligible for PrEP and deliver risk reduction and adherence counseling [50]. Solutions to these issues may be addressed by leveraging existing resources to provide PrEP services, including cross-training of staff (e.g., health educators, pharmacists, nurses) to deliver PrEP counseling [52]. Similar to the movement away from “HIV exceptionalism” and integration of routine HIV testing into primary care settings [53],[54], PrEP delivery will require integration into primary care settings to maximize PrEP coverage of at-risk individuals. Experience and lessons learned from PrEP implementation programs in more specialized settings (e.g., STD/HIV clinics) can be used to develop user-friendly tools (e.g., patient education and counseling materials, checklists for PrEP prescribing) to facilitate primary care providers delivering PrEP in their practices [50].
Optimize PrEP support
Promoting accurate risk perception and information about potential FTC/TDF side effects and strategies to cope with them will be critical to successful PrEP implementation. Risk assessment tools are currently being developed and validated [55],[56], and several PrEP demonstration projects are evaluating strategies such as text messaging to support adherence and promote retention [32]. Other programs are evaluating the role of real-time pharmacokinetic testing to monitor adherence and trigger enhanced adherence interventions. In The Demo Project, we have developed a one-page handout called “PrEP Basics,” which provides anticipatory guidance regarding PrEP use (see Text S1).
Combat PrEP stigma
Participants in the Demo Project and other PrEP studies have reported feeling stigmatized by their decision to use PrEP by medical providers, friends, and sex partners. HIV-related stigma and discrimination have a profoundly negative impact on people living with and at risk for HIV [57], acting as deterrents to HIV-testing, serostatus disclosure, and linkage and retention in care [58]. Likewise, PrEP-related stigma could act as an important barrier to PrEP uptake and dissemination. Combating PrEP stigma will require a multi-faceted approach, including social-marketing campaigns, education for health care providers, and a broad recognition of PrEP users as individuals proactively using proven prevention strategies.
Moving Forward
As the PrEP and HIV prevention fields evolve, several key questions will need to be addressed to optimize PrEP delivery. These issues include determining the optimal target populations for PrEP, standardizing guidelines for initiating and discontinuing PrEP, and evaluating cost-effectiveness. Our early experience with PrEP in San Francisco has illustrated that interest in PrEP is high among populations at risk for HIV infection, and PrEP can be incorporated into busy clinical settings. We believe PrEP can be an important component of comprehensive HIV prevention programs that include efforts to improve HIV testing, linkage to care, and early initiation of antiretroviral therapy.
Supporting Information
Zdroje
1. GrantRM, LamaJR, AndersonPL, McMahanV, LiuAY, et al. (2010) Preexposure chemoprophylaxis for HIV prevention in men who have sex with men. N Engl J Med 363 : 2587–2599.
2. Baeten JM, Donnell D, Ndase P, Mugo NR, Campbell, JD, et al.. (2012) Antiretroviral prophylaxis for HIV prevention in heterosexual men and women. N Engl J Med. 367: : 399–410.
3. ThigpenMC, KebaabetswePM, PaxtonLA, SmithDK, RoseCE, et al. (2012) Antiretroviral preexposure prophylaxis for heterosexual HIV transmission in Botswana. N Engl J Med 367 : 423–434.
4. ChoopanyaK, MartinM, SuntharasamaiP, SangkumU, MockPA, et al. (2013) Antiretroviral prophylaxis for HIV infection in injecting drug users in Bangkok, Thailand (the Bangkok Tenofovir Study): a randomised, double-blind, placebo-controlled phase 3 trial. Lancet 381 : 2083–2090.
5. KoenigLJ, LylesC, SmithDK (2013) Adherence to antiretroviral medications for HIV pre-exposure prophylaxis: lessons learned from trials and treatment studies. Am J Prev Med 44: S91–98.
6. MarcusJL, GliddenDV, MayerKH, LiuAY, BuchbinderSP, et al. (2013) No evidence of sexual risk compensation in the iPrEx trial of daily oral HIV preexposure prophylaxis. PLoS ONE 8: e81997.
7. LiuAY, VittinghoffE, ChillagK, MayerK, ThompsonM, et al. (2013) Sexual risk behavior among HIV-uninfected men who have sex with men participating in a tenofovir preexposure prophylaxis randomized trial in the United States. J Acquir Immune Defic Syndr 64 : 87–94.
8. SmithD, GrantR, WeidleP, LanskyA, MerminJ, et al. (2011) Interim guidance: preexposure prophylaxis for the prevention of HIV Infection in men who have sex with men. MMWR 60.
9. GomezGB, BorquezA, CaseKK, WheelockA, VassallA, et al. (2013) The cost and impact of scaling up pre-exposure prophylaxis for HIV prevention: a systematic review of cost-effectiveness modelling studies. PLoS Med 10: e1001401.
10. JuusolaJL, BrandeauML, OwensDK, BendavidE (2012) The cost-effectiveness of preexposure prophylaxis for HIV prevention in the United States in men who have sex with men. Ann Intern Med 156 : 541–550.
11. SchackmanBR, EggmanAA (2012) Cost-effectiveness of pre-exposure prophylaxis for HIV: a review. Curr Opin HIV AIDS 7 : 587–592.
12. Van DammeL, CorneliA, AhmedK, AgotK, LombaardJ, et al. (2012) Preexposure prophylaxis for HIV infection among African women. N Engl J Med 367 : 411–422.
13. Marrazzo J, Ramjee G, Nair G, Palanee T, Mkhize B, et al.. (2013) Pre-exposure prophylaxis for HIV in women: daily oral tenofovir, oral tenofovir/emtricitabine, or vaginal tenofovir gel in the VOICE Study (MTN 003). In: Proceedings of the 20th Conference on Retroviruses and Opportunistic Infections; 3–6 March 2013; Atlanta, Georgia, United States of America. Abstract 26LB.
14. ArnoldEA, HazeltonP, LaneT, ChristopoulosKA, GalindoGR, et al. (2012) A qualitative study of provider thoughts on implementing pre-exposure prophylaxis (PrEP) in clinical settings to prevent HIV infection. PLoS ONE 7: e40603.
15. SaberiP, GamarelKE, NeilandsTB, ComfortM, SheonN, et al. (2012) Ambiguity, ambivalence, and apprehensions of taking HIV-1 pre-exposure prophylaxis among male couples in San Francisco: a mixed methods study. PLoS ONE 7: e50061.
16. FuchsJD, SobieszczykME, MadenwaldT, GroveD, KarunaST, et al. (2013) Intentions to use preexposure prophylaxis among current phase 2B preventive HIV-1 vaccine efficacy trial participants. J Acquir Immune Defic Syndr 63 : 259–262.
17. KrakowerDS, MimiagaMJ, RosenbergerJG, NovakDS, MittyJA, et al. (2012) Limited awareness and low immediate uptake of pre-exposure prophylaxis among men who have sex with men using an internet social networking site. PLoS ONE 7: e33119.
18. van der StratenA, Van DammeL, HabererJE, BangsbergDR (2012) Unraveling the divergent results of pre-exposure prophylaxis trials for HIV prevention. AIDS 26: F13–19.
19. HurtCB, EronJJJr, CohenMS (2011) Pre-exposure prophylaxis and antiretroviral resistance: HIV prevention at a cost? Clin Infect Dis 53 : 1265–1270.
20. KurtzSP, ButtramME, SurrattHL (2013) Vulnerable infected populations and street markets for ARVs: potential implications for PrEP rollout in the USA. AIDS Care 26 : 411–415.
21. GolubSA, KowalczykW, WeinbergerCL, ParsonsJT (2010) Preexposure prophylaxis and predicted condom use among high-risk men who have sex with men. J Acquir Immune Defic Syndr 54 : 548–555.
22. HorbergM, RaymondB (2013) Financial policy issues for HIV pre-exposure prophylaxis: cost and access to insurance. Am J Prev Med 44: S125–128.
23. MyersJE, SepkowitzKA (2013) A pill for HIV prevention: deja vu all over again? Clin Infect Dis 56 : 1604–1612.
24. De ManJ, ColebundersR, FlorenceE, LagaM, KenyonC (2013) What is the place of pre-exposure prophylaxis in HIV prevention? AIDS Rev 15 : 102–111.
25. EakleR, VenterWD, ReesH (2013) Pre-exposure prophylaxis for HIV prevention: ready for prime time in South Africa? S Afr Med J 103 : 515–516.
26. GuptaRK, Van de VijverDA, ManicklalS, WainbergMA (2013) Evolving uses of oral reverse transcriptase inhibitors in the HIV-1 epidemic: from treatment to prevention. Retrovirology 10 : 82.
27. MolinaJM, PintadoC, GateyC, PonscarmeD, CharbonneauP, et al. (2013) Challenges and opportunities for oral pre-exposure prophylaxis in the prevention of HIV infection: where are we in Europe? BMC Med 11 : 186.
28. RennieS (2013) Ethical use of antiretroviral resources for HIV prevention in resource poor settings. Dev World Bioeth 13 : 79–86.
29. VenterF, AllaisL, RichterM (2013) Exposure ethics: does Hiv pre-exposure prophylaxis raise ethical problems for the health care provider and policy maker? Bioethics In press.
30. CohenMS, MuessigKE, SmithMK, PowersKA, KashubaAD (2012) Antiviral agents and HIV prevention: controversies, conflicts, and consensus. AIDS 26 : 1585–1598.
31. World Health Organization (2012) Guidance on pre-exposure oral prophylaxis (PrEP) for serodiscordant couples, men and transgender women who have sex with men at high risk of HIV: recommendations for use in the context of demonstration projects. Geneva: WHO.
32. BaetenJM, HabererJE, LiuAY, SistaN (2013) Preexposure prophylaxis for HIV prevention: where have we been and where are we going? J Acquir Immune Defic Syndr 63 (Suppl 2) S122–129.
33. Center for Disease Control and Prevention (2010) Prevalence and awareness of HIV infection among men who have sex with men — 21 cities, United States, 2008. MMWR Morb Mortal Wkly Rep 59 : 1201–1207.
34. San Francisco Department of Public Health (2013) HIV/AIDS Epidemiology Annual Report 2012. San Francisco: HIV Epidemiology Section.
35. BernsteinKT, MarcusJL, NieriG, PhilipSS, KlausnerJD (2010) Rectal gonorrhea and chlamydia reinfection is associated with increased risk of HIV seroconversion. J Acquir Immune Defic Syndr 53 : 537–543.
36. KatzMH, BrighamTM (2011) Transforming a traditional safety net into a coordinated care system: lessons from healthy San Francisco. Health Aff (Millwood) 30 : 237–245.
37. WeberS, WalduraJF, CohanD (2013) Safer conception options for HIV serodifferent couples in the United States: the experience of the National Perinatal HIV Hotline and Clinicians' Network. J Acquir Immune Defic Syndr 63: e140–141.
38. CohenSE, LiuAY, BernsteinKT, PhilipS (2013) Preparing for HIV pre-exposure prophylaxis: lessons learned from post-exposure prophylaxis. Am J Prev Med 44: S80–85.
39. LiuAY, KittredgePV, VittinghoffE, RaymondHF, AhrensK, et al. (2008) Limited knowledge and use of HIV post - and pre-exposure prophylaxis among gay and bisexual men. J Acquir Immune Defic Syndr 47 : 241–247.
40. CampbellJD, HerbstJH, KoppenhaverRT, SmithDK (2013) Antiretroviral prophylaxis for sexual and injection drug use acquisition of HIV. Am J Prev Med 44: S63–69.
41. Al-TayyibAA, ThrunMW, HaukoosJS, WallsNE (2013) Knowledge of pre-exposure prophylaxis (PrEP) for HIV prevention among men who have sex with men in Denver, Colorado. AIDS Behav In press.
42. My PrEP Experience Blogspot. Available: http://myprepexperience.blogspot.com/p/truvada-track.html. Accessed 26 September 2013.
43. Truvada for PrEP Medication Assistance Program. Available: http://gilead.com/responsibility/us-patient-access/truvada%20for%20prep%20medication%20assistance%20program. Accessed 25 June 2013.
44. KrakowerD, MayerKH (2012) Engaging healthcare providers to implement HIV pre-exposure prophylaxis. Curr Opin HIV AIDS 7 : 593–599.
45. BernsteinKT, LiuKL, BegierEM, KoblinB, KarpatiA, et al. (2008) Same-sex attraction disclosure to health care providers among New York City men who have sex with men: implications for HIV testing approaches. Arch Intern Med 168 : 1458–1464.
46. MimiagaMJ, GoldhammerH, BelanoffC, TetuAM, MayerKH (2007) Men who have sex with men: perceptions about sexual risk, HIV and sexually transmitted disease testing, and provider communication. Sex Transm Dis 34 : 113–119.
47. Centers for Disease Control, Prevention (1994) HIV prevention practices of primary-care physicians–United States, 1992. MMWR Morb Mortal Wkly Rep 42 : 988–992.
48. LoebDF, LeeRS, BinswangerIA, EllisonMC, AagaardEM (2011) Patient, resident physician, and visit factors associated with documentation of sexual history in the outpatient setting. J Gen Intern Med 26 : 887–893.
49. MontanoDE, PhillipsWR, KasprzykD, GreekA (2008) STD/HIV prevention practices among primary care clinicians: risk assessment, prevention counseling, and testing. Sex Transm Dis 35 : 154–166.
50. NortonWE, LarsonRS, DearingJW (2013) Primary care and public health partnerships for implementing pre-exposure prophylaxis. Am J Prev Med 44: S77–79.
51. HosekSG (2013) HIV pre-exposure prophylaxis diffusion and implementation issues in nonclinical settings. Am J Prev Med 44: S129–132.
52. BrunoC, SaberiP (2012) Pharmacists as providers of HIV pre-exposure prophylaxis. Int J Clin Pharm 34 : 803–806.
53. BayerR, FairchildAL (2006) Changing the paradigm for HIV testing–the end of exceptionalism. N Engl J Med 355 : 647–649.
54. SmithR, ZetolaNM, KlausnerJD (2007) Beyond the end of exceptionalism: integrating HIV testing into routine medical care and HIV prevention. Expert Rev Anti Infect Ther 5 : 581–589.
55. CelumC, BaetenJM, HughesJP, BarnabasR, LiuA, et al. (2013) Integrated strategies for combination HIV prevention: principles and examples for men who have sex with men in the Americas and heterosexual African populations. J Acquir Immune Defic Syndr 63 (Suppl 2) S213–220.
56. SmithDK, PalsSL, HerbstJH, ShindeS, CareyJW (2012) Development of a clinical screening index predictive of incident HIV infection among men who have sex with men in the United States. J Acquir Immune Defic Syndr 60 : 421–427.
57. MahajanAP, SaylesJN, PatelVA, RemienRH, SawiresSR, et al. (2008) Stigma in the HIV/AIDS epidemic: a review of the literature and recommendations for the way forward. AIDS 22 (Suppl 2) S67–79.
58. SmitPJ, BradyM, CarterM, FernandesR, LamoreL, et al. (2012) HIV-related stigma within communities of gay men: a literature review. AIDS Care 24 : 405–412.
Štítky
Interné lekárstvo
Článok vyšiel v časopisePLOS Medicine
Najčítanejšie tento týždeň
2014 Číslo 3- Parazitičtí červi v terapii Crohnovy choroby a dalších zánětlivých autoimunitních onemocnění
- Intermitentní hladovění v prevenci a léčbě chorob
- Statinová intolerance
- Co dělat při intoleranci statinů?
- Monoklonální protilátky v léčbě hyperlipidemií
-
Všetky články tohto čísla
- How Can Journals Respond to Threats of Libel Litigation?
- and Water, Sanitation, and Hygiene: A Committed Relationship
- Representation and Misrepresentation of Scientific Evidence in Contemporary Tobacco Regulation: A Review of Tobacco Industry Submissions to the UK Government Consultation on Standardised Packaging
- Building Research Capacity in Africa: Equity and Global Health Collaborations
- Associations between Intimate Partner Violence and Health among Men Who Have Sex with Men: A Systematic Review and Meta-Analysis
- Active or Passive Exposure to Tobacco Smoking and Allergic Rhinitis, Allergic Dermatitis, and Food Allergy in Adults and Children: A Systematic Review and Meta-Analysis
- The Effectiveness of Community Action in Reducing Risky Alcohol Consumption and Harm: A Cluster Randomised Controlled Trial
- Assessing Causality in the Association between Child Adiposity and Physical Activity Levels: A Mendelian Randomization Analysis
- The Impact of Pyrethroid Resistance on the Efficacy of Insecticide-Treated Bed Nets against African Anopheline Mosquitoes: Systematic Review and Meta-Analysis
- Lung Function and Incidence of Chronic Obstructive Pulmonary Disease after Improved Cooking Fuels and Kitchen Ventilation: A 9-Year Prospective Cohort Study
- Early Experiences Implementing Pre-exposure Prophylaxis (PrEP) for HIV Prevention in San Francisco
- The Role of Viral Introductions in Sustaining Community-Based HIV Epidemics in Rural Uganda: Evidence from Spatial Clustering, Phylogenetics, and Egocentric Transmission Models
- PLOS Medicine
- Archív čísel
- Aktuálne číslo
- Informácie o časopise
Najčítanejšie v tomto čísle- and Water, Sanitation, and Hygiene: A Committed Relationship
- Representation and Misrepresentation of Scientific Evidence in Contemporary Tobacco Regulation: A Review of Tobacco Industry Submissions to the UK Government Consultation on Standardised Packaging
- The Impact of Pyrethroid Resistance on the Efficacy of Insecticide-Treated Bed Nets against African Anopheline Mosquitoes: Systematic Review and Meta-Analysis
- The Role of Viral Introductions in Sustaining Community-Based HIV Epidemics in Rural Uganda: Evidence from Spatial Clustering, Phylogenetics, and Egocentric Transmission Models
Prihlásenie#ADS_BOTTOM_SCRIPTS#Zabudnuté hesloZadajte e-mailovú adresu, s ktorou ste vytvárali účet. Budú Vám na ňu zasielané informácie k nastaveniu nového hesla.
- Časopisy



