-
Články
- Časopisy
- Kurzy
- Témy
- Kongresy
- Videa
- Podcasty
Risk of Injurious Fall and Hip Fracture up to 26 y before the Diagnosis of Parkinson Disease: Nested Case–Control Studies in a Nationwide Cohort
In two nested case-control studies using data from a nationwide cohort, Peter Nordström and colleagues assess the risk of injurious fall and hip fracture up to 26 years before the diagnosis of Parkinson's disease.
Published in the journal: Risk of Injurious Fall and Hip Fracture up to 26 y before the Diagnosis of Parkinson Disease: Nested Case–Control Studies in a Nationwide Cohort. PLoS Med 13(2): e32767. doi:10.1371/journal.pmed.1001954
Category: Research Article
doi: https://doi.org/10.1371/journal.pmed.1001954Summary
In two nested case-control studies using data from a nationwide cohort, Peter Nordström and colleagues assess the risk of injurious fall and hip fracture up to 26 years before the diagnosis of Parkinson's disease.
Introduction
Fall-related injuries are a major cause of morbidity and mortality in the elderly population [1]. The risk of falling is increased in patients with Parkinson disease (PD) [2,3], and the incidence of hip fracture is particularly high [4], possibly due to dysfunctional balance reactions and impaired ability to protect the hip when falling [5].
PD has an insidious onset; the cardinal motor symptoms are preceded by substantial neurodegeneration [6,7], the timing of which remains uncertain [8,9]. Several studies have reported increased occurrence of nonspecific symptoms years or decades before the diagnosis of PD [8,9]. These prodromal signs reported typically do not involve motor function. Balance impairment has been considered to be a late-stage symptom in PD; it defines the transition to stage 3 on the Hoehn and Yahr scale [10]. However, this staging relies on the clinical evaluation of balance. Quantitative measurements of postural stability have detected abnormalities also in the early stages of PD [11,12], and recent findings suggest that balance can be impaired in the prodromal phase of the disease [13–15]. Whether such subclinical deficits increase the risk of falling remains unclear, but a high incidence of accidental injuries in the years preceding PD diagnosis has been reported [13]. In a recent investigation of the Swedish male population, we found lower muscle strength 30 y before the diagnosis of PD [16]. The effect size of the relation between muscle strength and PD was small, but an association between similarly subtle strength deficits and an increased risk of low-energy fractures has previously been reported [17]. We hypothesized that the reduced muscle strength found in our previous study might be a marker of neuromuscular dysfunction that could translate into an increased risk of falling and fractures a long time before PD diagnosis. Thus, the aim of the present study was to evaluate the risk of injurious falls prior to the clinical onset of PD from a long-term perspective. In a nationwide cohort consisting of all individuals aged ≥50 y, we identified those diagnosed with PD between 1988 and 2012. Using a nested case—control (NCC) design with attention to temporal perspectives, we investigated whether PD diagnosis was preceded by injurious falls in general, and by hip fracture in particular.
Methods
Study Population
Permission for the present study was granted by the local ethics committee of Umeå University. The assignment of a unique personal identification number to every Swedish citizen ensures that nationwide registers and databases are highly reliable. The National Patient Register (NPR) provides records of all public inpatient healthcare since 1987, and outpatient consultations in specialist clinics since 2001 [18]. Diagnoses are coded according to the Swedish versions of the International Classification of Diseases (ICD-9 in 1987–1997, ICD-10 since 1998), and the records have shown a high degree of validity, with positive predictive values of 85%–97% [19]. All residents of Sweden aged ≥50 y on December 31, 2005 (n = 3,329,400), were considered for inclusion in the present study. Personal identification numbers were used to link data from the NPR with those from other nationwide registers before encoding and depersonalization.
Diagnoses and Matched Cohort Definition
Within the cohort, we traced diagnoses of PD (ICD-9 code 332A, ICD-10 code G20.9) recorded in the NPR between January 1, 1987, and December 31, 2012. For the same period, we traced medical consultations and hospitalizations due to falls (ICD-9 code E885, ICD-10 codes W00 and W01). In these fall-related care events, we also captured diagnoses of the most common fractures (hip [ICD-9 code 820, ICD-10 codes S72.0–S72.2], wrist [ICD-9 code 813, ICD-10 code S52], lower leg [ICD-9 code 824, ICD-10 code S82], and humerus [ICD-9 code 812, ICD-10 codes S42.2–S42.4]) and head injuries (ICD-9 codes 800–804 and 850–853; ICD-10 codes I62, S02, and S06). Mortality data were obtained from the National Cause of Death Register.
Based on the information obtained, we compiled two NCC cohorts (Fig 1). Cohort I was compiled with the aim of analyzing the risk of falls and fractures prior to PD diagnosis compared with matched controls, with a retrospective design allowing capture of recurrent events. For this, each case of PD was matched by sex and year of birth to ten population-based controls, drawn from all residents of Sweden aged ≥50 y on December 31, 2005. The index date for each matched group was defined by the earliest recorded PD diagnosis. Controls deceased before the index date were excluded and were replaced when a new matching control who was alive on the index date could be found within three additional matching attempts. All individuals with index dates before January 1, 1988, were excluded from analyses, to provide a minimum retrospective study time of 1 y and to allow 1 y to capture diagnoses of PD in individuals with disease onset before data collection began.
Fig. 1. Selection process of the nested case—control cohorts. 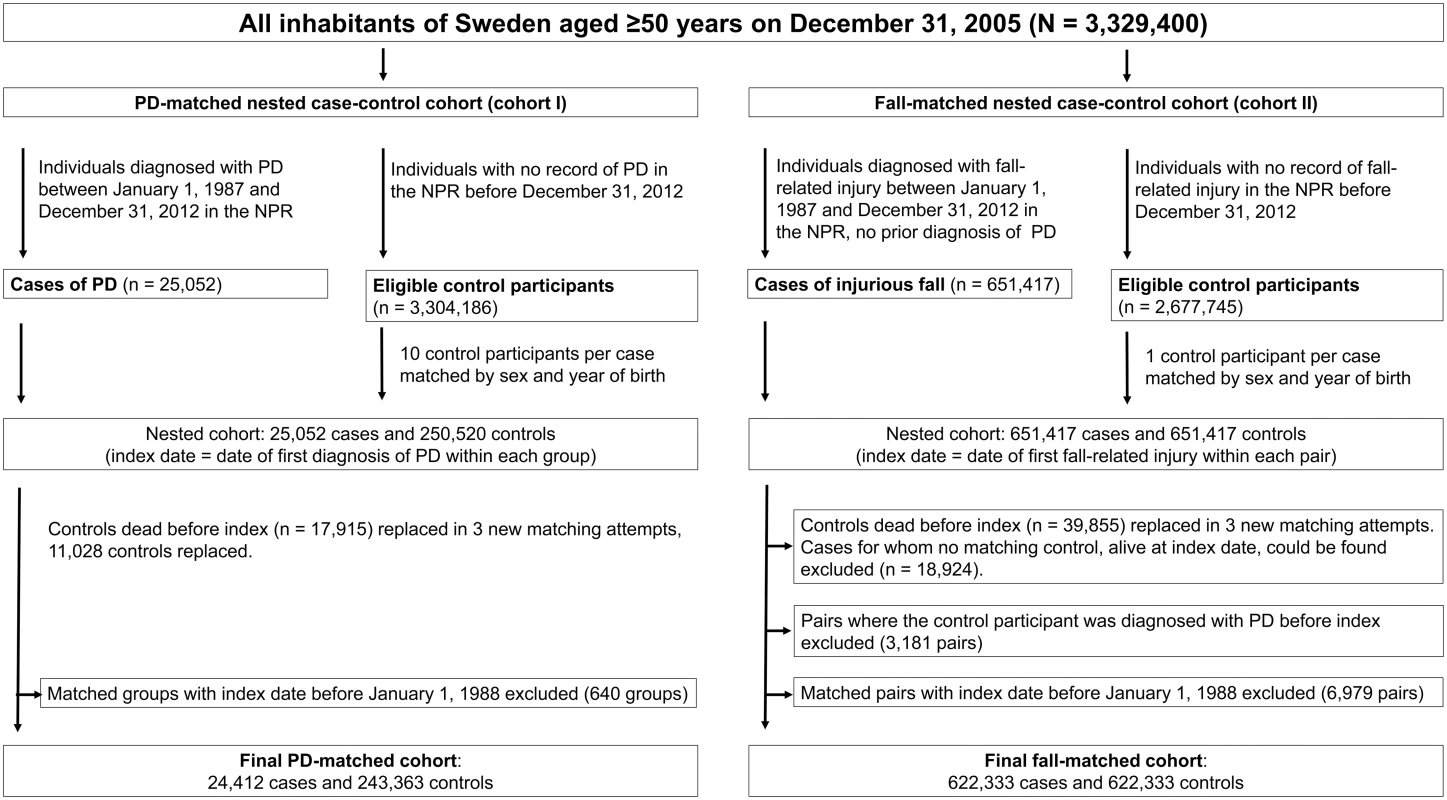
The second NCC cohort (cohort II) was compiled with the aim of prospectively evaluating the risk of PD after an injurious fall. Again, all residents of Sweden ≥50 y of age by the end of 2005 were considered for inclusion; each individual with a record of injurious fall not preceded by a PD diagnosis in the NPR was matched by sex and year of birth to one control with no record of fall-related injury, drawn from the same population. The index date for each matched pair was defined by the first recorded injurious fall, and pairs containing a control diagnosed with PD before the index date were excluded. Controls deceased before the index date were replaced when possible. Individuals with an injurious fall for whom no matching control alive on the index date could be found within three additional matching attempts were excluded. To allow for 1 y to capture diagnoses of PD, individuals with an index date for injurious fall before January 1, 1988, were excluded from analysis.
Additional Covariates
Other diagnoses that might confound the associations studied were selected as covariates based on previous known associations with falls [20,21] and were acquired from the NPR, including dementia (ICD-9 codes 290, 291, and 294B; ICD-10 codes F00, F01, F03.9, G30, G31, and E51.2), stroke (ICD-9 codes 431 and 434, ICD-10 codes I61–I64), myocardial infarction (ICD-9 code 410, ICD-10 codes I21 and I22), diabetes mellitus (ICD-9 code 250, ICD-10 codes E10 and E11), depression (ICD-9 code 311, ICD-10 codes F32 and F33), alcohol dependency or abuse (ICD-9 codes 303 and 305A, ICD-10 code F10), and drug dependency or abuse (ICD-9 codes 304 and 305X, ICD-10 codes F11–F19). As a proxy for socioeconomic situation, information about individuals’ education level (low, vocational school or ≤9 y of primary school; high, university or ≥3 y of secondary school) was obtained from the Statistics Sweden database; this information was available for 98.8% of individuals in cohort I and 97.8% of individuals in cohort II.
Statistical Analyses
Stata (version 13.1 for Windows; StataCorp) and SPSS (version 22.0 for Windows; SPSS Inc.) software packages were used for statistical analyses. Data are presented as valid percentages and medians with ranges, unless otherwise indicated. Chi-squared tests and Wilcoxon rank-sum tests were used for univariate analyses. p-Values less than 0.05 were considered significant.
In the PD-matched cohort (cohort I), the study time was calculated backward from the index date to January 1, 1987, and incidences of injurious fall and hip fracture were investigated in separate time intervals before the index date: 0 to <3 mo, 3 to <12 mo, 1 to <2 y, 2 to <3 y, 3 to <4 y, 4 to <5 y, 5 to <7 y, 7 to <10 y, 10 to <15 y, and 15 to <26 y before the index date (Fig 2). Medical consultations with aftercare diagnoses (ICD-9 codes V53, V54, and V58; ICD-10 codes Z09.4, Z47, Z48, Z50.8, and Z50.9) were excluded. Odds ratios (ORs) according to PD were calculated separately for each time interval and for each of the outcomes (injurious fall and hip fracture), using conditional logistic regression models adjusted for education level and comorbid diagnoses (and sex and year of birth by the statistical model).
Fig. 2. Overview of data collection and study times. 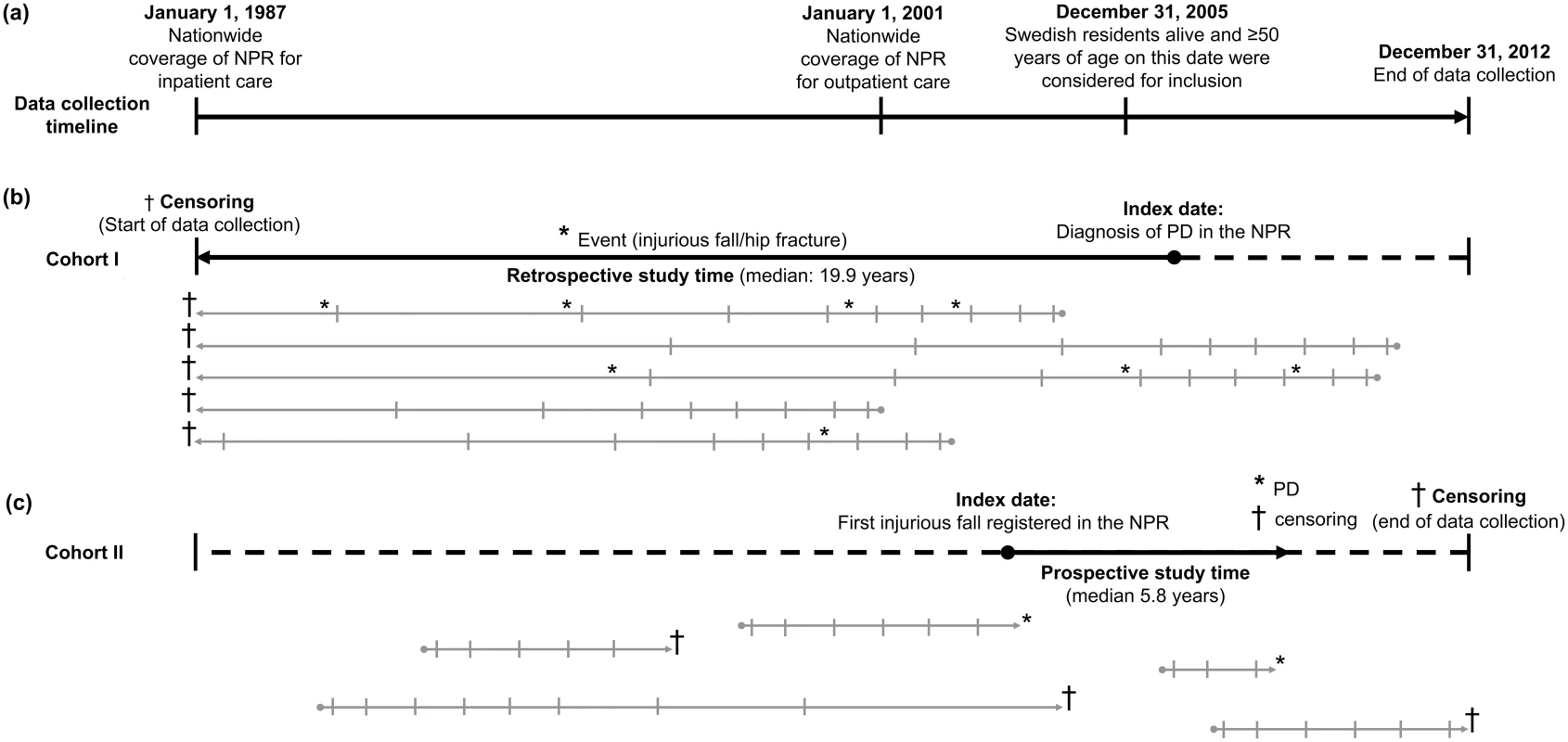
(A) The timeline of data collection according to calendar dates. (B) Retrospective analyses in cohort I. The gray arrows provide a schematic illustration of single individuals’ study time, with events (fall/hip fracture) marked (*) above the line. Left censoring (†) occurs at the beginning of the data collection time. Time intervals used in analyses are indicated by horizontal lines (0 to <3 mo, 3 to <12 mo, 1 to <2 y, 2 to <3 y, 3 to <4 y, 4 to <5 y, 5 to <7 y, 7 to <10 y, 10 to <15 y, and 15 to 26 y before the index date). (C) Prospective analyses in cohort II. Individual study times are indicated the same way as in (B), with the follow-up time split into the following intervals after the index date: 0 to <3 mo, 3 to <12 mo, 1 to <2 y, 2 to <3 y, 3 to <4 y, 4 to <5 y, 5 to <7 y, 7 to <10 y, 10 to <15 y, and 15 to 25 y. Marks above the arrow indicate PD (*) or censoring (†) due to death or end of data collection. In the fall-matched cohort (cohort II), the follow-up time was calculated from the index date to the date of PD, death, or December 31, 2012, whichever came first. We evaluated the proportional hazards assumption using a Cox model with Schoenfeld residuals and found that the association between injurious fall and subsequent PD did not meet the criteria for proportional hazards (χ2 = 156.2 at one degree of freedom; p < 0.001). Thus, we further analyzed this association using a flexible parametric Royston—Parmar model [22], allowing the relationship between the exposure and the outcome to vary over time. Individuals with a follow-up time of <3 mo were excluded. To test the consistency of the results, we assessed the ORs for PD in different time intervals using a conditional logistic regression model, as described above. The time intervals for this prospective analysis were 0 to <3 mo, 3 to <12 mo, 1 to <2 y, 2 to <3 y, 3 to <4 y, 4 to <5 y, 5 to <7 y, 7 to <10 y, 10 to <15 y, and 15 to 25 y after the index date. To assess potential confounding by the competing risk of death, we also performed the same analyses separately in a sub-cohort (cohort IIb) where all matched pairs in which either individual died during follow-up were excluded. All models were adjusted for sex and year of birth, education level, and comorbidities diagnosed before the index date.
Results
Descriptive data for the two NCC cohorts are presented in Table 1. Cohort I comprised 24,412 individuals with PD and 243,363 controls (47.1% women), with a median age of 75.4 y (range 32.0‒103.7) on the index date. During a median study period of 19.9 y (range 1.0–25.0) before the index date, 18.0% of individuals with PD and 11.5% of controls had at least one injurious fall (p < 0.001), resulting in at least one fracture in 10.7% of individuals with PD and 6.9% of controls (p < 0.001). The incidence of hip fracture prior to the index date was 7.1% and 3.2%, respectively, among individuals with PD and controls (p < 0.001; Table 1).
Tab. 1. Descriptive data of the case—control cohorts. 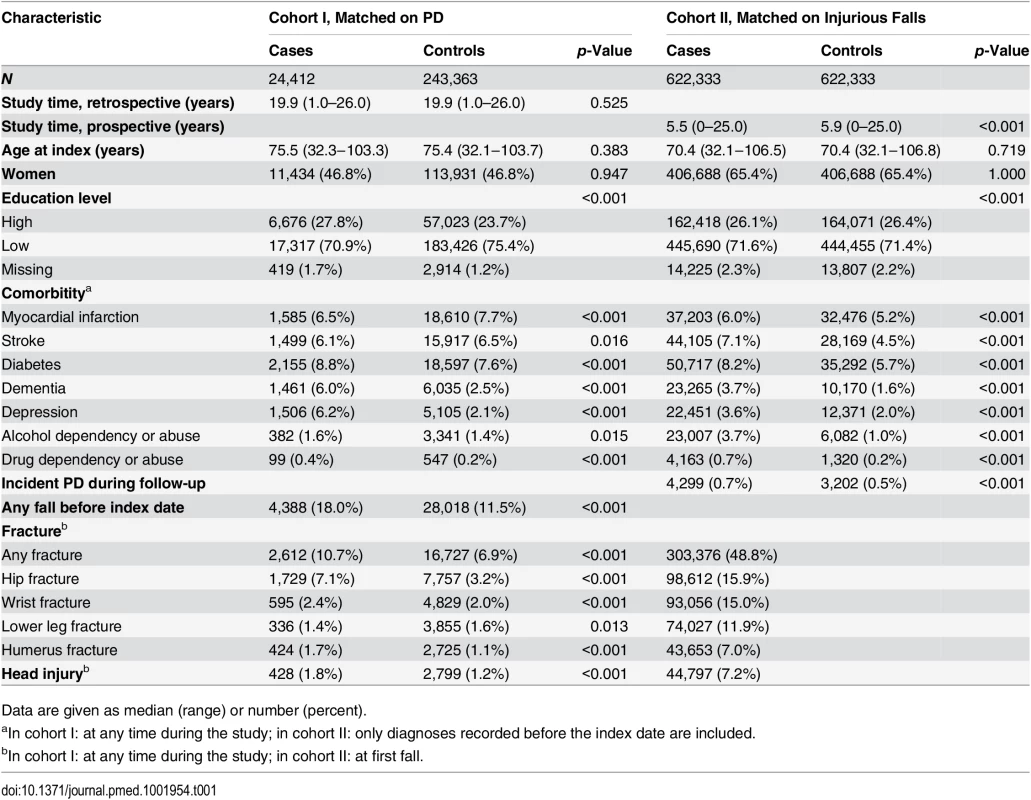
Data are given as median (range) or number (percent). In the multivariable adjusted analyses of cohort I (Table 2), an elevated risk of falls appeared in the decade before PD diagnosis (OR 1.19, 95% CI 1.08–1.31; 7 to <10 y before diagnosis, for cases versus controls), and the association was further accentuated closer to the index date (OR 1.94, 95% CI 1.79–2.11; 3 to <12 mo before diagnosis). The association between PD and hip fracture was even stronger, with an approximately 2-fold increased risk in all intervals between 3 mo and <4 y prior to PD diagnosis, and this association was significant ≥15 y before diagnosis (OR 1.36, 95% CI 1.10–1.69; 15 to 26 y before PD diagnosis). In the last 3 mo before PD diagnosis, the ORs for injurious fall and for hip fracture increased distinctly, to 5.83 (95% CI 5.30–6.42) for falls and 7.49 (95% CI 6.52–8.61) for hip fracture, for individuals with PD versus controls.
Tab. 2. Incidence and odds ratios of injurious fall and hip fracture in cohort I. 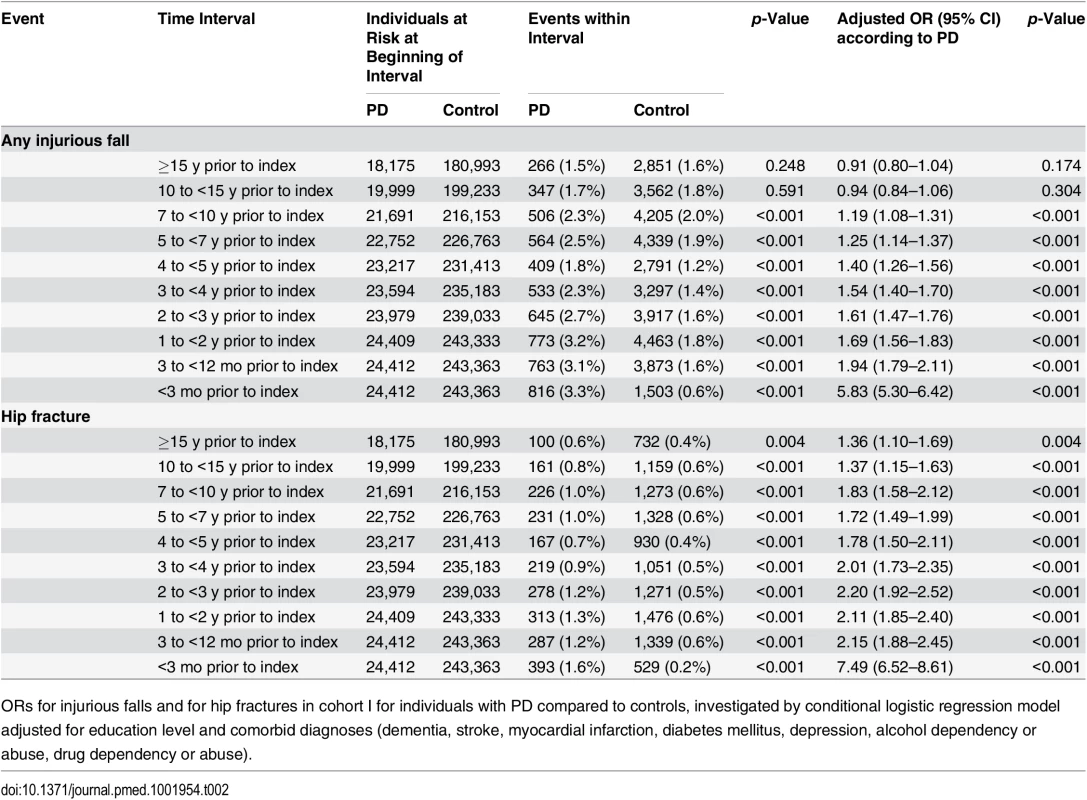
ORs for injurious falls and for hip fractures in cohort I for individuals with PD compared to controls, investigated by conditional logistic regression model adjusted for education level and comorbid diagnoses (dementia, stroke, myocardial infarction, diabetes mellitus, depression, alcohol dependency or abuse, drug dependency or abuse). Results of the prospective sensitivity analyses of risk of PD after injurious fall in cohort II are presented in Fig 3 (Royston—Parmar model) and Table 3 (conditional logistic regression). Cohort II consisted of 622,333 individuals with an injurious fall and 622,333 individuals without an injurious fall (65.4% women) with a median age of 70.4 y (range 32.1‒106.8) at the time of the first registered injurious fall. The most common fall-related injuries were fractures of the hip (15.9%), wrist (15.0%), lower leg (11.9%), and humerus (7.0%). During the follow-up period (median 5.8 y, range 0–25.0), 7,501 (0.6%) individuals in this cohort were diagnosed with PD (4,299 [0.7%] individuals with an injurious fall, 3,202 [0.5%] controls; p < 0.001; Table 1).
Fig. 3. Hazard ratio for Parkinson disease according to fall in cohort II. 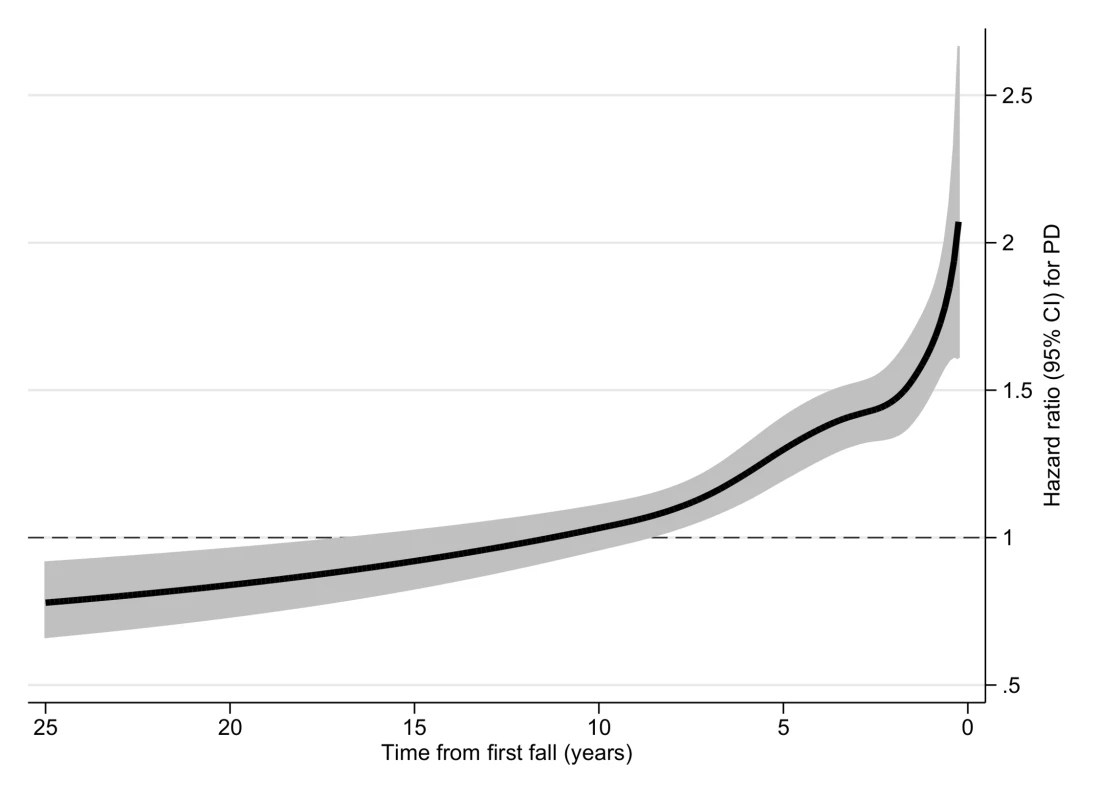
Hazard ratio for PD after first injurious fall in cohort II, estimated by a flexible parametric Royston—Parmar model adjusted for sex, year of birth, education level, and comorbid diagnoses (dementia, stroke, myocardial infarction, diabetes mellitus, depression, alcohol dependency or abuse, drug dependency or abuse). The gray areas represent the 95% confidence intervals. Tab. 3. Incidence of Parkinson disease according to fall in cohort II. 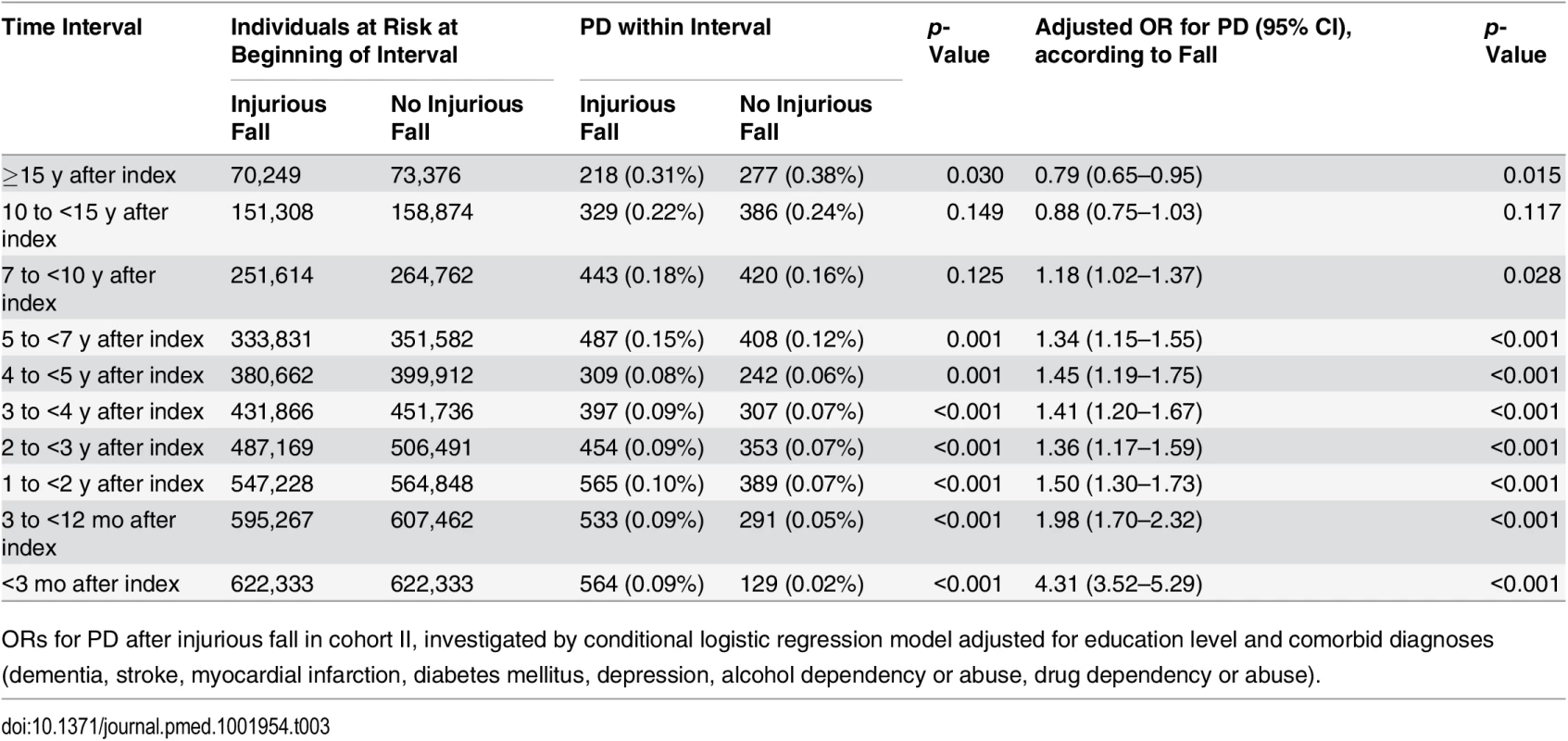
ORs for PD after injurious fall in cohort II, investigated by conditional logistic regression model adjusted for education level and comorbid diagnoses (dementia, stroke, myocardial infarction, diabetes mellitus, depression, alcohol dependency or abuse, drug dependency or abuse). Assessed by the Royston—Parmar model, the risk of PD was elevated among individuals with an injurious fall during the first ~10 y of study enrollment and then appeared to decrease significantly compared with controls at follow-up times ≥15 y (Fig 3). Regression analyses confirmed these findings, with ORs declining from 1.98 (95% CI 1.70–2.32) at 3 to <12 mo after the first fall to 0.79 (95% CI 0.65–0.95) at ≥15 y after the first fall (Table 3). However, in the sub-cohort excluding all pairs censored by death (S1 Table), no inverse relationship between falling and PD was observed (S2 Table; S1 Fig).
Discussion
To our knowledge, this study is the first long-term investigation of fall risk prior to the clinical onset of PD. In general, we found that the risk of injurious falls was elevated a decade before the diagnosis of PD, and the risk of hip fracture was increased ≥15 y before the diagnosis of PD. The strength of these associations between injurious falls, hip fracture, and PD increased distinctly up to the diagnosis of PD. The time-dependent patterns indicate a direct link between injurious falls and subsequent PD, and may be explained by subtle neurodegenerative impairment many years before the diagnosis of this disease.
In the present study, diagnoses of dementia, depression, and diabetes were more common in PD cases than in controls, which may have contributed to the higher risk of falls before the index date [20,21]. Irrespectively of this, a recent study from the UK revealed that balance impairment was more common up to 5 y prior to diagnosis in individuals diagnosed with PD compared to controls [14]. This finding is particularly noteworthy, as postural imbalance is not expected to be clinically overt until the later stages of PD [11,23]. Moreover, given that subclinical deficits in postural stability have been noted in early PD [11,12], similar findings of increased postural sway in patients with rapid eye movement sleep behavior disorder may indicate balance impairments in prodromal PD, as more than half of these patients are expected to eventually develop parkinsonism (PD, multiple system atrophy, or Lewy body dementia) [15]. Such subtle deficits could conceivably translate into increased risks of falling and consequent injury in prodromal PD, but, to our knowledge, only one previous study [13] has addressed this question. The authors reported an increased incidence of accidental injury prior to PD but included data from only the last 3 y of the prodromal phase [13], whereas our results indicate an association with hip fracture decades before diagnosis.
The results of the present study are supported by previous findings of low hand-grip and elbow-flexion strength three decades before the diagnosis of PD [16]. The involvement of the upper extremity is of particular interest in relation to the increased risk of hip fracture in the present study, as dysfunctional arm movements when falling are thought to play an important role in the high incidence of hip fracture in patients with PD [2]. Thus, taken together, our present and previous [16] findings may indicate that such deficits arise long before the cardinal signs of PD become overt.
Some limitations of the present study should be noted. First, data were obtained from registers, and diagnoses could not be clinically confirmed for the present study, although all diagnoses were recorded in the context of specialist healthcare. Compared to residents of urban areas, individuals with PD in rural parts of Sweden may be less likely to be diagnosed in specialist health care, and therefore less likely to be included as cases of PD in the present study. A similar effect could be expected for fall-related injuries; less severe injuries that do not demand surgery are less likely to be diagnosed in specialist care. Thus, the accuracy for hip fractures can be expected to be higher than for fall-related injuries in general [24]. Any incorrect or missed diagnosis would contribute to regression dilution bias, causing wider standard errors and attenuation of the associations found between PD and injurious falls toward zero [25]. Second, the observational nature of this study did not permit exploration of the mechanisms underlying the observed associations or documentation of a causal link between injurious falls and PD, although the time-dependent associations found strongly suggest such a relationship. Third, we lacked information about smoking status. This would have been of interest since smoking is associated with a reduced risk for PD [26]. Having a higher education level is known to be associated with less smoking [27,28], and smoking status may therefore explain the association between higher education and PD in the present study. The main strengths of the present study include the large body of prospectively recorded data covering a long period, which provided superior statistical power for the performance of reliable analyses from a long-term perspective and which was not subject to recall bias. The main results of the present study were also evaluated in cohort II, and the findings were consistent. Thus, the sensitivity analysis supported the validity of the main findings, and because the individuals were drawn from a nationwide cohort, the external validity of the results is likely high.
In conclusion, we found that the risk of injurious falls in general, and especially those resulting in hip fracture, was increased decades before the diagnosis of PD. These findings suggest that clinically relevant neurodegenerative impairment could be present many years before the clinical onset of the disease. It would be of value if our results identifying markers of PD more than a decade before diagnosis, from the present and previous studies [16,29], could be confirmed in other settings and in other countries.
Supporting Information
Zdroje
1. Kannus P, Sievänen H, Palvanen M, Järvinen T, Parkkari J. Prevention of falls and consequent injuries in elderly people. Lancet. 2005;366 : 1885–1893. doi: 10.1016/s0140-6736(05)67604-0 16310556
2. Grimbergen YA, Munneke M, Bloem BR. Falls in Parkinson’s disease. Curr Opin Neurol. 2004;17 : 405–415. 15247535
3. Pickering RM, Grimbergen YA, Rigney U, Ashburn A, Mazibrada G, Wood B, et al. A meta-analysis of six prospective studies of falling in Parkinson’s disease. Mov Disord. 2007;22 : 1892–1900. doi: 10.1002/mds.21598 17588236
4. Lyell V, Henderson E, Devine M, Gregson C. Assessment and management of fracture risk in patients with Parkinson’s disease. Age Ageing. 2015;44 : 34–41. doi: 10.1093/ageing/afu122 25236847
5. Carpenter MG, Allum JH, Honegger F, Adkin AL, Bloem BR. Postural abnormalities to multidirectional stance perturbations in Parkinson’s disease. J Neurol Neurosurg Psychiatry. 2004;75 : 1245–1254. doi: 10.1136/jnnp.2003.021147 15314109
6. Fearnley JM, Lees AJ. Ageing and Parkinson’s disease: substantia nigra regional selectivity. Brain. 1991;114(Pt 5):2283–2301. 1933245
7. Marek K, Jennings D. Can we image premotor Parkinson disease? Neurology. 2009;72(7 Suppl):S21–S26. doi: 10.1212/WNL.0b013e318198df97 19221310
8. Hawkes CH, Del Tredici K, Braak H. A timeline for Parkinson’s disease. Parkinsonism Relat Disord. 2010;16 : 79–84. doi: 10.1016/j.parkreldis.2009.08.007 19846332
9. Savica R, Rocca WA, Ahlskog JE. When does Parkinson disease start? Arch Neurol. 2010;67 : 798–801. doi: 10.1001/archneurol.2010.135 20625084
10. Hoehn MM, Yahr MD. Parkinsonism: onset, progression and mortality. Neurology. 1967;17 : 427–442. 6067254
11. Beuter A, Hernandez R, Rigal R, Modolo J, Blanchet PJ. Postural sway and effect of levodopa in early Parkinson’s disease. Can J Neurol Sci. 2008;35 : 65–68. 18380279
12. Mancini M, Horak FB, Zampieri C, Carlson-Kuhta P, Nutt JG, Chiari L. Trunk accelerometry reveals postural instability in untreated Parkinson’s disease. Parkinsonism Relat Disord. 2011;17 : 557–562. doi: 10.1016/j.parkreldis.2011.05.010 21641263
13. Frandsen R, Kjellberg J, Ibsen R, Jennum P. Morbidity in early Parkinson’s disease and prior to diagnosis. Brain Behav. 2014;4 : 446–452. doi: 10.1002/brb3.228 24944873
14. Schrag A, Horsfall L, Walters K, Noyce A, Petersen I. Prediagnostic presentations of Parkinson’s disease in primary care: a case—control study. Lancet Neurol. 2015;14 : 57–64. doi: 10.1016/s1474-4422(14)70287-x 25435387
15. Chen TZ, Xu GJ, Zhou GA, Wang JR, Chan P, Du YF. Postural sway in idiopathic rapid eye movement sleep behavior disorder: a potential marker of prodromal Parkinson’s disease. Brain Res. 2014;1559 : 26–32. 24602694
16. Gustafsson H, Aasly J, Stråhle S, Nordström A, Nordström P. Low muscle strength in late adolescence and Parkinson disease later in life. Neurology. 2015;84 : 1862–1869. doi: 10.1212/WNL.0000000000001534 25841033
17. Nordström P, Sievänen H, Gustafson Y, Pedersen NL, Nordström A. High physical fitness in young adulthood reduces the risk of fractures later in life in men: a nationwide cohort study. J Bone Miner Res. 2013;28 : 1061–1067. doi: 10.1002/jbmr.1829 23184669
18. Swedish National Board of Health and Welfare. The National Patient Register. Available: http://www.socialstyrelsen.se/register/halsodataregister/patientregistret/inenglish. Accessed 26 Apr 2015.
19. Ludvigsson JF, Andersson E, Ekbom A, Feychting M, Kim JL, Reuterwall C, et al. External review and validation of the Swedish national inpatient register. BMC Public Health. 2011;11 : 450. doi: 10.1186/1471-2458-11-450 21658213
20. Deandrea S, Lucenteforte E, Bravi F, Foschi R, La Vecchia C, Negri E. Risk factors for falls in community-dwelling older people: a systematic review and meta-analysis. Epidemiology. 2010;21 : 658–668. 20585256
21. Sattin RW. Falls among older persons: a public health perspective. Annu Rev Public Health. 1992;13 : 489–508. 1599600
22. Royston P, Parmar MK. Flexible parametric proportional-hazards and proportional-odds models for censored survival data, with application to prognostic modelling and estimation of treatment effects. Stat Med. 2002;21 : 2175–2197. doi: 10.1002/sim.1203 12210632
23. Jankovic J. Parkinson’s disease: clinical features and diagnosis. J Neurol Neurosurg Psychiatry. 2008;79 : 368–376. doi: 10.1136/jnnp.2007.131045 18344392
24. Michaelsson K, Baron JA, Farahmand BY, Johnell O, Magnusson C, Persson PG, et al. Hormone replacement therapy and risk of hip fracture: population based case—control study. The Swedish Hip Fracture Study Group. BMJ. 1998;316 : 1858–1863. 9632404
25. Hutcheon JA, Chiolero A, Hanley JA. Random measurement error and regression dilution bias. BMJ. 2010;340:c2289. doi: 10.1136/bmj.c2289 20573762
26. Hernan MA, Takkouche B, Caamano-Isorna F, Gestal-Otero JJ. A meta-analysis of coffee drinking, cigarette smoking, and the risk of Parkinson’s disease. Ann Neurol. 2002;52 : 276–284. doi: 10.1002/ana.10277 12205639
27. Giskes K, Kunst AE, Benach J, Borrell C, Costa G, Dahl E, et al. Trends in smoking behaviour between 1985 and 2000 in nine European countries by education. J Epidemiol Community Health. 2005;59 : 395–401. doi: 10.1136/jech.2004.025684 15831689
28. Cavelaars AE, Kunst AE, Geurts JJ, Crialesi R, Grotvedt L, Helmert U, et al. Educational differences in smoking: international comparison. BMJ. 2000;320 : 1102–1107. 10775217
29. Gustafsson H, Nordström A, Nordström P. Depression and subsequent risk of Parkinson disease: a nationwide cohort study. Neurology. 2015;84 : 2422–2429. doi: 10.1212/WNL.0000000000001684 25995056
Štítky
Interné lekárstvo
Článek 2015 Reviewer Thank You
Článok vyšiel v časopisePLOS Medicine
Najčítanejšie tento týždeň
2016 Číslo 2- Parazitičtí červi v terapii Crohnovy choroby a dalších zánětlivých autoimunitních onemocnění
- Intermitentní hladovění v prevenci a léčbě chorob
- Statinová intolerance
- Co dělat při intoleranci statinů?
- Metabolit živočišné stravy produkovaný střevní mikroflórou zvyšuje riziko závažných kardiovaskulárních příhod
-
Všetky články tohto čísla
- 2015 Reviewer Thank You
- The Future of Diabetes Prevention: A Call for Papers
- The Case for Reforming Drug Naming: Should Brand Name Trademark Protections Expire upon Generic Entry?
- The Health Care Consequences Of Australian Immigration Policies
- Microenvironmental Heterogeneity Parallels Breast Cancer Progression: A Histology–Genomic Integration Analysis
- Hand, Foot, and Mouth Disease in China: Modeling Epidemic Dynamics of Enterovirus Serotypes and Implications for Vaccination
- Estimated Effects of Different Alcohol Taxation and Price Policies on Health Inequalities: A Mathematical Modelling Study
- Effect of Short-Term Supplementation with Ready-to-Use Therapeutic Food or Micronutrients for Children after Illness for Prevention of Malnutrition: A Randomised Controlled Trial in Uganda
- Effect of Short-Term Supplementation with Ready-to-Use Therapeutic Food or Micronutrients for Children after Illness for Prevention of Malnutrition: A Randomised Controlled Trial in Nigeria
- When Children Become Adults: Should Biobanks Re-Contact?
- Transforming Living Kidney Donation with a Comprehensive Strategy
- A Time for Global Action: Addressing Girls’ Menstrual Hygiene Management Needs in Schools
- The Rise of Consumer Health Wearables: Promises and Barriers
- Risk of Injurious Fall and Hip Fracture up to 26 y before the Diagnosis of Parkinson Disease: Nested Case–Control Studies in a Nationwide Cohort
- Mortality, Morbidity, and Developmental Outcomes in Infants Born to Women Who Received Either Mefloquine or Sulfadoxine-Pyrimethamine as Intermittent Preventive Treatment of Malaria in Pregnancy: A Cohort Study
- PLOS Medicine
- Archív čísel
- Aktuálne číslo
- Informácie o časopise
Najčítanejšie v tomto čísle- Hand, Foot, and Mouth Disease in China: Modeling Epidemic Dynamics of Enterovirus Serotypes and Implications for Vaccination
- A Time for Global Action: Addressing Girls’ Menstrual Hygiene Management Needs in Schools
- Transforming Living Kidney Donation with a Comprehensive Strategy
- The Rise of Consumer Health Wearables: Promises and Barriers
Prihlásenie#ADS_BOTTOM_SCRIPTS#Zabudnuté hesloZadajte e-mailovú adresu, s ktorou ste vytvárali účet. Budú Vám na ňu zasielané informácie k nastaveniu nového hesla.
- Časopisy



